Fluoride: What to Use and When!
May 14, 2019
Who are we to tell our patients they can’t use something that we know may reverse a type of disease they have been diagnosed with.
This week I will talk about fluoride: What to use and when to use it.
WHAT IS FLUORIDE?
So, you may be one of the healthcare professionals who think fluoride is harmful.
I used to drink a lot of milk as a child. It was so much milk that my parents told me they would have to buy a cow. Can I drink milk as an adult? Am I lactose intolerant?
The answer is a bold, YES!
I overdosed on milk and now I am lactose intolerant.
So is it possible fluoride is a poison?
Yes, if too much is ingested on a regular basis. Fluoride can be very toxic if too much is ingested in a small period of time.
Fluoride is a naturally occurring element found in our soil but if not used properly it can cause serious medical problems.
OUR ROLE
I believe that we have a responsibility to treat each patient with a customized, individualized plan of care.
WHEN TO USE
In last week’s blog, I shared the latest CAMERA update and I invite you to refer to this when you have a patient who is at high-risk for caries. When you look at this information you will have a template that outlines “who” is at risk for caries.
WHICH FLUORIDE TO USE
There are many choices of fluoride to use so I will provide a brief overview of the most widely use, as well as, the latest on Silver Diamine Fluoride.
ACIDULATED PHOSPHATE FLUORIDE
This fluoride is also known as APF 1.23% and contains 12,300 ppm fluoride ion and it comes in foam and gel.
Please be aware that in 2013 the ADA Council on Scientific Affairs chairside recommendation’s advise against the use of 1.23% (APF) foam. The reason for this is that the research has not demonstrated its efficacy for caries prevention,
The benefits of using this fluoride are storage, stability, acceptable taste and tissue biocompatibility.
APF needs to remain in contact with the teeth for 4 minutes.
This can make administration more difficult for small children who have trouble sitting still in a dental chair. For this reason, children under 6 years of age should receive a fluoride varnish.
NEUTRAL SODIUM FLUORIDE
This gel was not included in the ADA Council on Scientific Affairs guidelines for caries prevention but it is still available for topically applied fluoride use.
The gel and foam have a ph of 7.o. A 2.0% Sodium Fluoride gel or foam has 9.050 ppm fluoride ion. Very much like APF, neutral sodium fluoride has good bioavailability and people find the taste pleasant.
Fluoride varnish is a highly is a highly concentrated form of sodium fluoride. 5% sodium fluoride varnish contains 22,600 ppm of fluoride ion.
Fluoride varnish was originally approved by the US Food and Drug Administration for the treatment of hypersensitivity but is used off-label for caries prevention.
The Cochrane Review states that patients treated with a fluoride varnish experienced an average reduction of 43% in carious lesions, less missing teeth and tooth restorations.
When looking at the effect on newly erupted or deciduous teeth the Cochrane Review discovered a 37% reduction in decayed, missing and tooth surfaces with restorations.
This is my personal choice when applying fluoride and it is what I recommend our clients use for their patients who are high-risk for caries and for children who qualify for a fluoride treatment.
The delivery of fluoride varnish allows the fluoride to remain in contact with the teeth for an extended amount of time.
Depending upon the patients’ risk for caries, fluoride varnish can be applied 2 to 4 times a year by a dental professional.
There is little evidence of adverse reactions to fluoride varnish placement and patients (especially younger children) are accepting of this preventie service.
From a personal point of communication, I share a story with patients, about living in Oregon and we MUST apply a varnish to our back deck or the wood will rot due to all the rain we receive in Oregon.
Use the example of the wood on a deck rotting when varnish is not applied. Explain that saliva has chemicals and possibly an unbalanced ph that will make the teeth rot. Applying the fluoride varnish will prevent the rot in teeth
Sounds corny? Sounds cheesy? Well, patients get it!
When you talk to patients about application of fluoride and/ or using fluoride at bedtime, talk about the cost benefit.
Explain that to have a fluoride varnish in the office two times a year and buying the take home fluoride gel may cost “X” but if the teeth need restorative services it now costs “x, y and z.”
Show your patients the plaque, the biofilm that is causing the carious lesions. Show your patients where decalcification areas are located and explain the benefits of prevention.
Explain that prevention costs less than treating disease (tooth decay; a cavity). Show your patient areas of root exposure and crown margins which at some point may have a carious lesion (cavity).
Showing patients is very helpful in getting them to make the change needed to prevent decay, use the fluoride, pay for what they want.
As the saying goes, “Seeing is believing!”
Also, check the ADA Codes when submitting for insurance reimbursement of the fluoride varnish.
I see it all the time that offices are using an old CDT code and therefore they don’t receive reimbursement or the highest dollar amount that can be reimbursed.
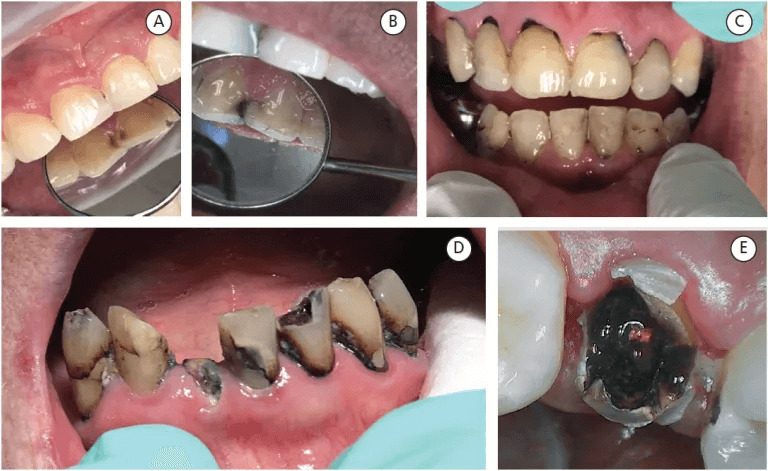
SILVER DIAMINE FLUORIDE
Silver diamine fluoride (SDF) is a combination of sodium fluoride and silver nitrate. Silver nitrate has been known for years as an antimicrobial agent. Sodium fluoride is known to reduce caries.
Sodium nitrate has the ability to arrest and prevent caries due to silver nitrate’s potent germicidal effect and fluoride’s ability to reduce decay. SDF is available in liquid concentration of 38.3% or 43.2%.
SDF is also approved for hypersensitivity and is used off label for caries management.
CONCLUSION
As healthcare professionals we have a responsibility to our patients to understand the value of the various types of fluoride. We must also know the indications for when to use each type of fluoride.
The best care we can provide our patients will be individualized and customized for their needs.
If you were asked, “Is this the best service you have to prevent cavities in my teeth?” what will your answer be?
ABOUT DEBBIE SEDIEL-BITTKE, RDH, BS
Debbie Seidel-Bittke, RDH, BS is founder and CEO of Dental Practice Solutions. Debbie is also a former dental hygiene program director. Her expertise is optimizing the hygiene department by taking a total team approach; including the doctor as the leader. Our Dental Practice University will launch for dentists and their team on June 6, 2019.
We are looking for ten offices to test drive (Beta-test) the university. The Dental Practice University has training video modules, forms and scripts for each department in your dental practice.
*For our beta-testers this includes modules for the doctor(s) about creating a culture to have a lot of new patients, keep your dental team the life-time of your dental practice, as well as re-create or create your vision and mission. Doctors receive a 90-Day goal setting journal.
The hygienists have their own training video modules that cover time management, caries risk, treating the gingivitis and periodontal patient.
The front office has video modules on phone calls, new patient calls, we provide job descriptions and a lot of information for hiring and keeping employees long- term.
You receive 24 AGD CE Credits. Once the University is open to all dental practices around the world, it will be FREE for the first 2 weeks and then $97.00 a month indefinitely. It includes AGD CE Credits for up to 2 employees each month. Additional employees can register and get the AGD CE Credits for $20/month.
If you would like to test drive the University over the next year, we do have a few requirements. Please text our office: 949-3551-8741 AND write DPU. You must include: YOUR NAME, YOUR DENTAL PRACTICE NAME, BEST PHONE NUMBER and EMAIL.
Once we receive this we will get back to you to discuss if you qualify for the “test drive” to Beta Test the Dental Practice University.
P.S. If you are chosen to test drive the DPU, two of your team members will receive the 24 AGD CE Credits.*